|
Getting your Trinity Audio player ready...
|
OWN VOICE. ~ InPerspective by Gregg Dieguez and Bruce Laird.
Note: Click on any chart to enlarge.
The Bottom Line:
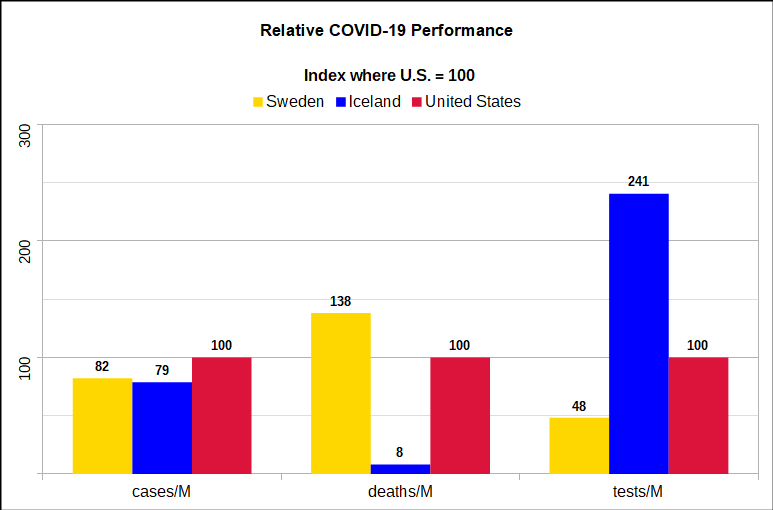
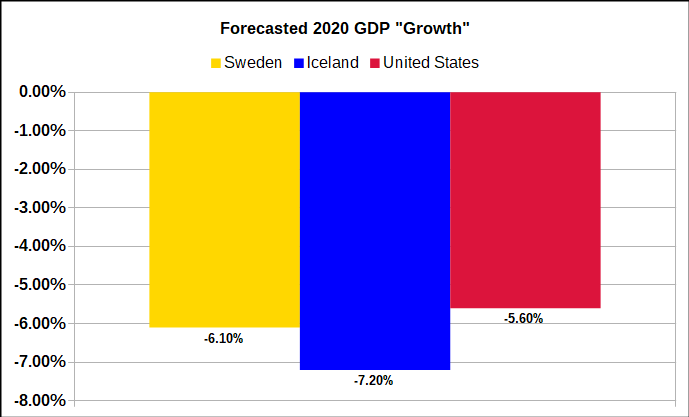
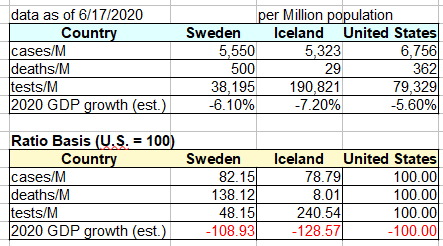
Iceland has roughly the same proportion of COVID-19 cases as Sweden or the United States, but a level of deaths per million that is less than one tenth of those countries. The chart at right [2] shows Sweden and Iceland compared to the U.S. with the US statistics per million indexed at 100. The U.S. has 20% more cases than either. Iceland has only 8% of the deaths per million compared with the U.S. Sweden has 17 times as many deaths as Iceland, and 38% more than the U.S. On the downside, Iceland is estimated to be contracting more in 2020 GDP than Sweden or the U.S., particularly because of its dependence on tourism (chart below)[3]. Nonetheless, we likely would have accepted 1.6% less GDP in exchange for saving 110,000 lives – which would have been our result – had we achieved Iceland’s level of Pandemic response.
So, how did Iceland accomplish such a low CV-19 death rate?
Different Strokes:
Sweden’s Approach:
To review, Sweden did NOT fully shut down, though they took several measures to control CV-19 spread:
1. Restricting travel & halting immigration
2. Banning gatherings of over 50 people
3. Instituting safety norms (hand washing, distance, work at home)
4. Asking older persons to stay home.
5. Closed secondary schools & universities
6. Working from home.
Sweden left bars and restaurants open. Their hope was that economic and mental health damage would be reduced, and that normally responsible Swedes would prevent massive spread of CV-19. Further, as in the U.S., the Swedish government didn’t have complete power to enforce a lockdown. Sweden’s initial economic damage has been FAR LESS than the U.S., but by year end, the U.S. is forecasted to recover strongly. To one expert, the Swedish model is an intriguing experiment in relying on the voluntary efforts of citizens to change their behaviors without severe mandates — and it is not going well. Sweden is 5th worst in deaths per million, and trending higher in cases.
Iceland’s Approach:
Iceland never imposed a lockdown, or even masks, but took the following measures:
1. Restricted travel in[4]
2. Banned gatherings above 20 people, at the start, no longer.
3. Extensive Testing
4. Thorough Contact Tracing
5. Quarantining contacts of those infected
6. Closed only bars, hair salons
7. Closed secondary schools & universities
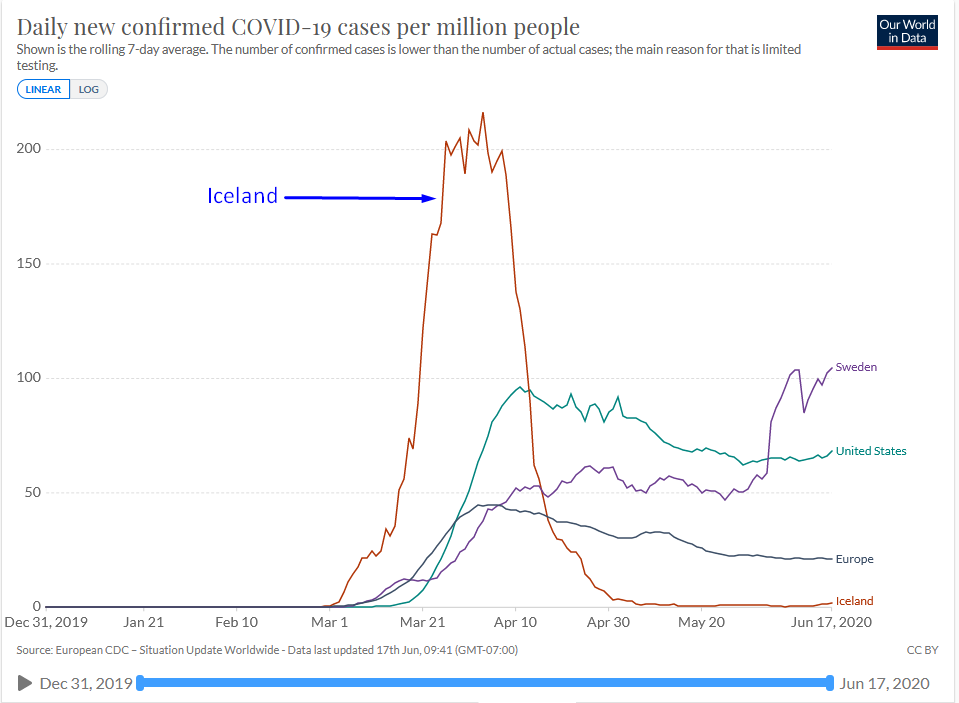
These policies initially resulted in more rapid spreading. In fact, in the early days of the outbreak, things looked very grim for Iceland. So how did Iceland manage to turn this around so successfully? The short answer is: they did it by following the classic epidemiology playbook: testing, isolation, relentless contact tracing, and mandatory 14-day quarantine for all viral contacts. Crucially, all Icelanders played by those rules. As it says on Iceland’s official COVID website, “Contagion tracing is a community affair.”
The graph at right shows the rapid increase in daily cases in Iceland, compared to other countries. Followed by a rapid decline to very low levels. The data are normalized to cases per million, for fair comparison.
Relentless Contact Tracing and Rigorous Quarantine
An excellent article in the New Yorker by Elizabeth Kolbert provides the detective story: Iceland’s first case was diagnosed on 28 Feb. The patient was a native Icelander, who returned home from a ski trip to the Dolomites, in Italy.
“[He was] back in Iceland for several days before he’d been diagnosed. During that time, he’d done all the things people normally do—gone to work, met with colleagues, run errands. Anyone who’d spent more than fifteen minutes near the man in the days before he’d experienced his first symptoms was considered potentially infected. (“Near” was defined as within a radius of two metres, or just over six feet.) The CT team came up with a list of fifty-six names. By midnight, all fifty-six contacts had been located and ordered to quarantine themselves for fourteen days.”
“The first case was followed by three more cases, then by six, and then by an onslaught. By mid-March, confirmed COVID cases in Iceland were increasing at a rate of sixty, seventy, even a hundred a day. As a proportion of the country’s population, this was far faster than the rate at which cases in the United States were growing. The number of people the tracing team was tracking down, meanwhile, was rising even more quickly. An infected person might have been near five other people, or fifty-six, or more. One young woman was so active before she tested positive—going to classes, rehearsing a play, attending choir practice—that her contacts numbered close to two hundred. All were sent into quarantine.”
“To find people who had been exposed, team members scanned airplane manifests and security-camera footage. They tried to pinpoint who was sitting next to whom on buses and in lecture halls. If you were returning to Iceland from overseas, you also got a call: put yourself in quarantine.”
As of June 17th, Iceland has 1,816 confirmed cases. But their CT process has resulted in 22,112 individuals entering 14-day quarantines. That’s a ratio of about 12 in quarantine for every confirmed case. Quarantining is a good part of the price that Icelanders paid for keeping their economy mostly open.
Extensive Testing
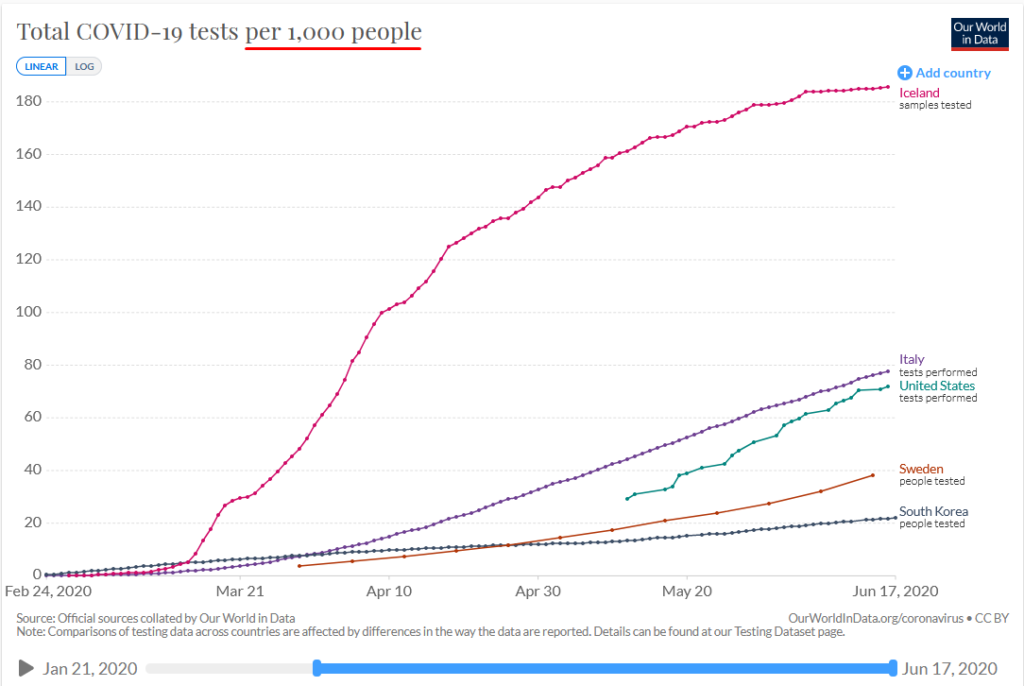
The graph below shows the rapid increase in testing in Iceland, compared to other countries. On a per capita basis, Iceland has the highest rate of testing in the world.
As of June 17, Iceland has administered 65,101 tests. Not a large number in absolute terms, but this equals testing 1 in 5 Icelanders. For Contact Tracing, Iceland has employed about 100 staff, including contact tracers, police detectives, and volunteers to make phone follow-ups, especially to the elderly. This team traced and sent over 22,112 Icelanders into fourteen-day quarantines (6.5% of population), 812 of those people are still there.
Quarantine Compliance and Follow-up
According to Kolbert, almost everyone in Iceland is at least distantly related to everyone else. Because of their comparatively homogeneous culture, Icelanders see themselves as one extended community, so they have complied with even the most extensive quarantine demands. When someone is instructed to isolate after testing positive, or required to quarantine because of contact with a positive case, that is only the beginning of the process. The infected who are not seriously ill are asked to isolate at home, to avoid crushing the hospitals. But there is daily follow-up to insure that if their symptoms worsen, they are immediately admitted to hospital. For those in quarantine, there are follow-up phone calls 2-3 times per week to determine if any of these people need to be tested and treated. In addition, many volunteers make daily wellness checks on all those over age 70, regardless of their quarantine status.
Implications for the United States
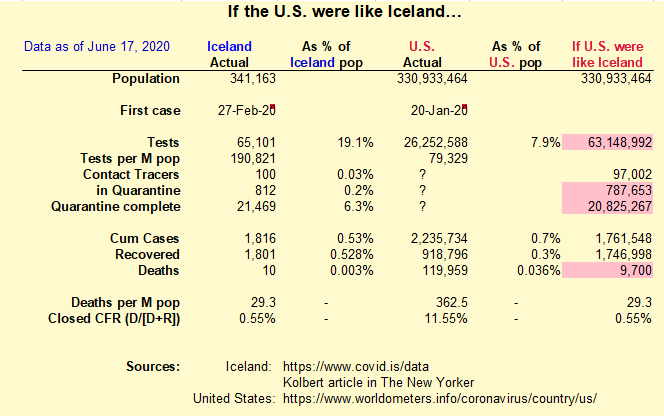
What U.S. effort would have been required to duplicate Iceland’s successful response? Our U.S. population is roughly 1,000 times that of Iceland. So to match the scale of the Icelandic effort we would have had to do 63 million tests to date. In fact, within 60 days of their first case on Feb 27., Iceland had tested 13.7% of their population. In the U.S., our first documented case was on Jan. 20th Equivalent performance would be if we had tested 45 million people by Mar. 20th. As of today, 5 months after our first confirmed case, the U.S. has tested only 26 million. Our testing – even with an earlier start in virus detection and after months to catch up – is only 41% of what would have been required for Iceland’s Detection-focused approach.
In addition, we would have had to quickly stand up a virtual team of at least 97,000 contact tracers nationwide, and quarantine 21.5 million citizens. Had the U.S. done that, our cumulative case total would have been 1.75 million (a 20% reduction). And crucially, we would have had under 10,000 deaths (!!). That’s a savings of 110,000 lives, or 91.7% of our fatalities, and counting. In addition, we would have been able to save much of the economic devastation we continue to experience.
There has been a lot of media coverage about the U.S. de-funding of critical epidemic preparedness resources in recent years; ignoring the early warnings of our public health experts; delayed and stumbling efforts to scale up testing; hobbling of our national health agencies and infrastructure by politics and lack of leadership. And most of all, media coverage of the tens of thousands of needless deaths and millions of jobs lost. We won’t attempt to repeat the details of those failings here. But even now, five months into the Pandemic, we have not managed to fully put in place the required testing, tracing and quarantine capabilities needed for the kind of success that Iceland (and several other countries) has achieved.
Clearly, the U.S. is not 1,000 Icelands. We are a much more heterogeneous nation of many cultures and beliefs, a supposed strength of our society. Because we lacked (and refused) early testing capabilities and CT infrastructure, we were left with the remaining Sophie’s Choice between extended economic harm or massive fatalities. Going forward, as we continue to be challenged, will we learn to act selflessly, as Icelanders have done? Or will our balkanized sense of individualism and entitlement continue to leave the U.S. the 7th worst country in CV-19 deaths per million?
Coming Soon:
We’ll have more articles shortly comparing different countries in their approach to COVID-19, and identifying the factors driving success or failure, as well as contrasts with U.S. performance.
FOOTNOTES:
[1] Of those countries whose measurements can be trusted, that is….
[2] Data Sources for Bar Charts
Data as of June 17th:
[3] Sources of GDP estimates:
Sweden: https://www.statista.com/statistics/1102546/coronavirus-european-gdp-growth/
Iceland: https://www.nordeatrade.com/se/explore-new-market/iceland/economical-context
United States: https://www.cbo.gov/publication/56335
Frankly, the way things are going lately in the U.S., I don’t trust the economy to have the foundation of trust in our mutual health necessary to ‘bounce back’ with any vigor, but I’m not an economist, so I’m using published forecasts. I fully expect to write an article in a few months (if I survive) titled “The Worst of Both Worlds”, showing BOTH U.S. CV-19 and economic performance as dismal.
[4] Icelandic Travel:
Note travelers must self-isolate for 14 days on arrival. Iceland GDP will depend largely on tourism: https://www.weforum.org/agenda/2020/05/iceland-tourism-covid19-tests/
More From Gregg Dieguez ~ “InPerspective”
Mr. Dieguez is a semi-successful, semi-retired MIT entrepreneur who causes occasional controversy Coastside. He lives in Montara. He loves to respond to comments. Mr. Laird is another semi-successful, semi-retired MIT entrepreneur but with more degrees, living in Los Altos. They roomed and caused trouble together back in the day.